By Maev Creaven Nutritional Therapist & Functional Medicine Practioner Speciality: Autoimmune, Digestive Health, Weight, Skin, Fatigue.
Oestrogen appears to play a central role in the immune response but can too much of it be a good thing?
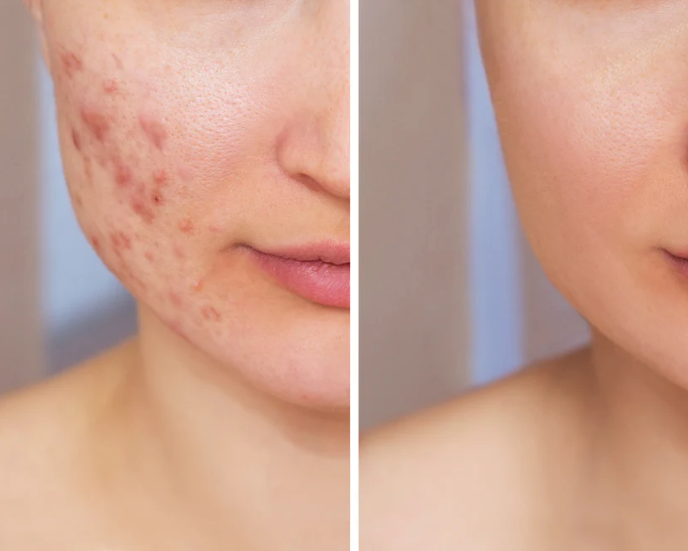
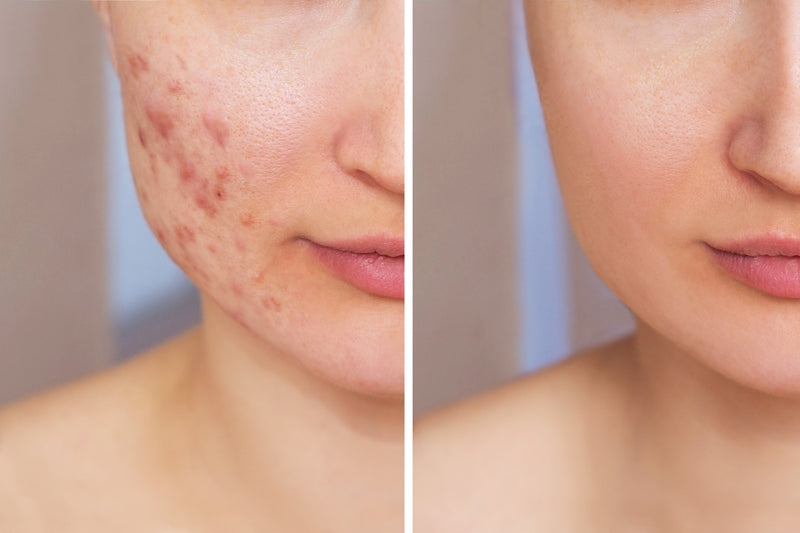
When clients come to me with hormonal imbalances or symptoms that range from oily skin and acne, digestive upset, PMS, or heavy, painful periods, the digestion and liver are two of the first areas we address. The liver is key to metabolism, detoxification, nutrient absorption, blood sugar balance, and immune system function. It is quite the superhero of the body.
Do you worry about your hormones? Maybe it’s a mild concern annoyingly sitting at the back of your mind from a niggling thought, period issues to (peri)menopause or beyond. Reducing risks for anything health related is always helpful. So what can we do to reduce risk around a hormonal related concern. Female hormones very much work in symphony and an imbalance in one hormone impacts another hormone's effectiveness.
Oestrogen levels fluctuate throughout life, naturally increasing during puberty and pregnancy and falling after menopause. During the menstrual cycle, oestrogen levels peak during ovulation dropping off if pregnancy does not occur. Abnormal oestrogen levels (too high or too low) can have a number of negative effects on health and wellbeing. Men also produce and require oestrogen for the maturation of sperm and a healthy libido but at significantly lower levels.
Oestrogen Dominance
High levels of oestrogen in relation to progesterone (testosterone in men) is known as oestrogen dominance and is becoming an increasingly common problem due to modern diet, lifestyle and environmental factors.
Do you know the signs of high oestrogen?
For women, symptoms range from PMS to heavy clots, increased body fat percentage, fibrocystic breasts, enlarged breasts, sexual dysfunction, fibroids, endometriosis, & mood issues (swings, depression, anxiety) brain fog, insomnia and more⠀
For men, symptoms present such as enlarged breasts (gynecomastia or man boobs), sexual dysfunction and / or infertility.
Oestrogen Deficiency
On the flip side oestrogen deficiency due to natural menopause or surgical menopause has been suggested to have an adverse effect on insulin resistance & fat distribution. Also low oestrogen is also common after coming off the birth control pill.
From the age of 40 onwards, oestrogen naturally drops off. With too little oestrogen, you may notice your skin thins or becomes more dry, dryness and thinning of the vagina, reduced / no periods, , and you probably don’t have much of a libido.
Low levels for men can present with excess belly fat and a low sex drive.
Too little oestrogen may be a sign you need more dietary fat. It is important to know what the right types of fats are for your genetics and health goals.
Oestrogen plays a vital role in bone, heart & skin health. However from all the essential functions oestrogen performs in the body, one of the most critical is optimising the action of insulin, the hormone that regulates blood sugar levels. Therefore, low oestrogen levels may lead to increased insulin resistance or impaired insulin action. Signs varies of insulin impairment and excess belly fat is one.
If you have a few ‘oestrogen type’ symptoms, you might want to have a conversation with your primary care doctor or your Nutritional Therapist.
Some of the most common contributors to oestrogen/progesterone imbalance are:
- Hormone Disruptors & Xenoestrogens
- Obesity
- Genetic Predisposition
- Gut Dysbiosis
- Diet
- Adrenal Dysfunction
As a Nutritional Therapist, I focus first on diet, detoxification and gut health, however the other common contributors tie in organically.
Elimination and Detoxification
There are three main phases to oestrogen detoxification. Two phases primarily involve your liver and the third phase, involves excretion via your kidneys or intestines to include bowel health and microbiome. For some that present with oestrogen dominance they could have issues with any combination of these phases.
I sometimes advise testing to know which phase is ‘off’ through either a hormonal panel or a microbiome / digestive test , this is really helpful, however there are many things you can start doing right now.
As mentioned, the main way your body eliminates oestrogen is through your bowel. If you have sluggish elimination, you may not get rid of oestrogen through the digestive tract. If oestrogen is not being eliminated through the bowel, it has a good opportunity to be reabsorbed and recycled back into the bloodstream (not a good thing!). There are many root causes that signal to a slow intestinal motility, hence why it’s important to work closely with a professional to personalise the approach, as no two women are the same!
I will share with you some dietary tips below tips, however it is just as important to address any nutrient imbalances such as low digestive enzymes or low stomach acid however there are many more (too many to get into for this short article).
If you don’t have enough digestive enzymes or stomach acid which are both quite common, your food will not be broken down enough for a smooth move through the intestines. When food moves slowly, bacteria have the chance to eat, proliferate and grow, which can offset the balance of your gut microbes.
Gut Bacteria and Hormones
When your gut bacteria is off or imbalanced, owing to low stomach acid, antibiotics, heavy metal exposure, excess sugar or a million other causes, it can affect the nerves that tell your intestines to contract and relax and move things along. So, an imbalanced gut both causes symptoms like IBS and SIBO (small intestinal bacterial overgrowth) – more on SIBO in another post, with the main symptoms are bloating, gas wind, or reflux, and more.
Finding the ‘root cause’ of these things can be frustrating, but if you suspect you have stomach acid or microbiome imbalances, ask your healthcare practitioner first for help, order some tests, but you could request supplementing with betaine HCl or digestive enzymes.
Also certain plants and nutrients may encourage the production of the enzymes involved in oestrogen metabolism and may support a healthy gut. Gut microbes can have a profound effect on hormones, especially oestrogen. Scientists refer to this connection between oestrogen and the microbiome as the “oestrobolome.” The oestrobolome is the bacteria associated with oestrogen metabolism and oestrogen levels.
Diet and lifestyle
Supporting your microbiome is effective in addressing female hormone dysregulation and it starts with your diet. Diet and lifestyle factors are commonly known to disrupt the gut microbiome and also have the potential to disrupt the oestrobolome. Emerging research indicates that the gut microbiome plays a central role in the regulation of oestrogen levels within the body and influences the risk of developing oestrogen-related diseases such as endometriosis, PCOS, and other hormonal metabolic diseases.
Below are some tips I recommend clients for a healthy gut and support of oestrogen metabolism:
- Keep it simple: Follow a diet rich in plant based nutrients, good quality proteins and adequate carbohydrates (subject to clients metabolic status).
- Add in plenty of liver-loving foods, for example eat a combination of these items weekly or preferably 1 cup a day: artichokes, beets, broccoli, brussels sprouts, cabbage, carrots cauliflower, garlic ,grapefruit, kale, onions, turmeric root
- Add in sulphur rich foods daily: garlic, onions, leeks, chives, cruciferous root vegetables.
- B12 is not found in vegetarian / vegan diets and may need to get tested and supplement accordingly
- Green leafy vegetables to be eaten in abundance, wild rocket, spinach etc. However, most vegetables have limitless benefits. For a good diversity of your bacteria in the gut (microbiome), try and bring in a broad range of vegetables to all meals.
- Quality protein sources. Most women I see in the clinic are not eating enough protein. Eat good quality proteins on a daily basis, like oily fish (wild is possible!), Irish beef, free-range poultry, pastured eggs and more!
- Increase magnesium rich foods, all green veg! Magnesium is the cofactor in the methylation detoxification pathway for oestrogen. Magnesium with B6 helps to reduce PMS symptoms.
- Eat foods with good bacteria (homemade yoghurt, sauerkraut).
- Olive oil: choose a good quality source. Olive oil contains a high level of anti-inflammatory activity due to its’ natural antioxidant called hydroxytyrosol (a polyphenol). Oils such as vegetable, corn, peanut, and soy are pro-inflammatory sources of omega 6 essential fatty acids, which tend to be over used by most people. Omega 6’s are not bad, they simply need to be kept in balance with the amount of omegas 3’s we eat, and they must also not be overheated in cooking.
- Wild blueberries and brightly coloured vegetables: These are all foods that have a high level of phytonutrients. If a vegetable [or fruit] is bright in colour, this implies that there is a high level of antioxidants present, which act as natural anti-inflammatories. Wild blueberries have an extremely high ORAC* [Oxygen Radical Absorbance Capacity) value .
- Cacao: This is a well loved nut and the main ingredient in chocolate. Raw cacao beans have an antioxidant score (ORAC*) of 95,500. To put that into perspective, that’s 14 times more antioxidant flavonoids than red wine, and 7 times more than even dark chocolate!
- Cinnamon has an ORAC* value of 267,536*. Cinnamon is well published to help reduce blood sugars, which means for some people it helps reduce cravings and the need for more sugar in the diet.
- Antioxidant and fibre foods. These include vegetables, nuts, seeds and berries. Fibre can help cleanse the colon, curb hunger, support your metabolism and balance hormones. Fibrous foods contain lots of antioxidants, such as leafy greens or berries, are also beneficial because of their ability to decrease free radical damage (which ages skin).
- Water: Yes, it’s not a food, but it needs a mention. Many experts suggest you drink around 8 glasses per day, but this is completely dependent on the amount of sweating and exercise you partake in daily. Dehydration can lead to bloating and dry skin, try to eat more naturally hydrating foods. These include fresh veggies and fruit, especially melon, berries, cucumber, celery, citrus fruits and fresh herbs.
- Flaxseeds. Flax is great for skin health and losing weight as can modulate oestrogen levels and may also increase collagen production. You can sprinkle flax on your breakfast, in your smoothies or simply eat the seeds by themselves.
- Potassium-rich foods. Flushing excess fluids and waste out of cells can help reduce cellulite. Green leafy vegetables, avocados, bananas, coconut water and cultured dairy are all high in potassium.
- Some of my favourite plant nutrients for hormones are sage, rosemary, selenium. Sage is a useful culinary herb in menopause as found to reduce hot flushes
- Healthy fats (EFAs and MCFAs). Did you know all of our hormones come from fats? Fats do not make you fat. Coconut and wild-caught fish contain fatty acids that promote healthy tissue.
What Not to Eat
- Goes without saying to reduce or avoid alcohols, sugars or sweeteners. Not only is poor sugar control a significant stressor on the body, but chronically high blood glucose and or insulin levels directly affect hormones.
- As much as possible avoid eating overcooked meat (browned of blackened ie BBQ), this contains PAHs that encourage production of carcinogens. However, if you marinate meat in advance this offsets the PAHs.
- Processed grains and cereals: breakfast cereals are often highly refined and full of added sugar (think insulin and insulin resistance! ).
- Also intensively farmed dairy and meats are not good quality either! These can be high in arachidonic acids, which can increase inflammatory biproducts.
The list goes on, but my preference is always to add in good quality foods, rather than focusing on restriction.
Finally, I wish to point out whether you are low or high oestrogen or progesterone etc, the functional medicine model is not about supplementing or giving medication for that specific hormone. It is focused on determining the underlying cause of the problem and addressing it at that level, and then once you do that, the hormones self-regulate and take care of themselves. If in doubt, test don't guess!
Let food and lifestyle be your medicine.
Advanced Testing
Did you know you can test your microbiome and evaluate certain markers that may help support your hormonal balance. Available at Nuala Woulfe Salon with our Nutritional Therapist (Functional Medicine) Maev Creaven. Take the guest work out and focus on your diet with a tailored plan.
- Complete hormonal panel
- Comprehensive Nutrient Panel
- Comprehensive Digestive Panel
We would like to hear from you. Is there a particular subject you would like covered in our next newsletter.
Maev Creaven
Nutritional Therapist, Functional Medicine Practitioner
Instagram: @maevcreaven
Facebook: www.facebook.com/maevcreavennutrition
Terms used in this article:
- Insulin resistance (IR) is associated with metabolic syndrome; a medical condition that can increase the risk of health problems like diabetes, cardiovascular disease and stroke. ⠀
-
Oestrogen is the name for the collective group of metabolites which play a major function in women’s reproductive function,⠀
and a minor one in males. There are three major forms of oestrogenoestrone (E1), oestradiol (E2) the most active oestrogen, oestriol (E3) is a weaker form on route to excretion.⠀